International Journal of Periodontics & Restorative Dentistry, Pre-Print
DOI: 10.11607/prd.6453, PubMed-ID: 3781985111. Okt. 2023,Sprache: EnglischGiudice, Amerigo / Attanasio, Ferdinando / Bennardo, Francesco / Antonelli, Alessandro / Vercellotti, Tomaso
The management of marked horizontal bone atrophy represents a critical challenge for traditional implantology procedures. For this purpose, clinicians have developed several protocols and procedure to allow the most suitable and accurate surgical and prosthetic implant rehabilitation. Despite the development of guided-bone regeneration methods or the use of small-diameter implants, the rehabilitation of thin bone areas represents a clinical dilemma for the medium- and long-term survival of implant-prosthetic therapies. This clinical case evaluates the use of wedge implants for the full arch rehabilitation of an atrophic maxilla with a thin ridge. This treatment choice allowed a minimally invasive rehabilitation, avoiding regenerative bone surgery, while respecting biological and prosthetic limits. Furthermore, the evaluation of ISQ and MBL values during the first year of follow-up allowed us to analyse the behaviour of this rehabilitation solution in full arch maxillary cases.
Implantologie, 2/2021
Seiten: 131-142, Sprache: DeutschVercellotti, Tomaso
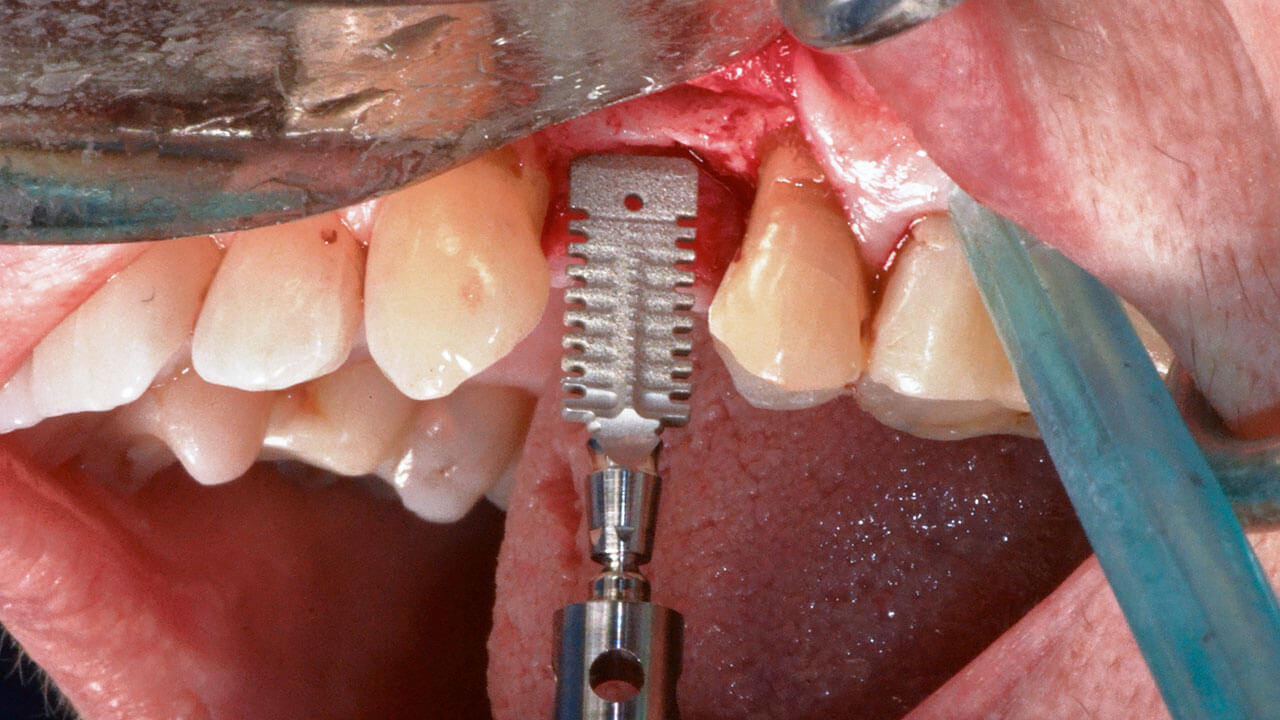
Schmale Knochenkämme sind ein häufiges Problem in der oralen Implantologie. Bei Vorliegen eines horizontalen Knochendefektes ist das Einsetzen eines Implantats nach alleiniger Implantatbettpräparation ohne vorherigen Knochenaufbau häufig nicht möglich, da eine adäquate vestibuläre und orale Knochendicke um das Implantat nicht sichergestellt ist. Die mindestens erforderliche Kammbreite, um ein Zylinder- oder Konusimplantat mit Standarddurchmesser inserieren zu können, liegt bei ungefähr 6,0 mm. Ist die Kammbreite geringer, muss eine Knochenaugmentation vorgenommen werden. Diese erhöht jedoch die Invasivität, Komplexität, Morbidität und Behandlungsdauer sowie die Therapiekosten. In diesem Beitrag soll ein neuartiges, keilförmiges Implantat mit schlankem rechteckigem Querschnitt eingeführt werden, das eine minimalinvasive Implantatsetzung in schmale Knochenkämme ermöglicht. Neben den klinischen Überlegungen hinter der Entwicklung und Konstruktion von keilförmigen Implantaten liefert dieser Beitrag ein Schritt-für-Schritt-Protokoll der neuen Techniken für die Implantatbettpräparation, die elektronisch gesteuert und ausschließlich mit piezoelektrischen Instrumenten und neuen Instrumenten für die Kammexpansion durchgeführt wird. Beschrieben werden ein Fall, in dem ein keilförmiges Implantat in einem einzeitigen Verfahren in einen Restkamm mit 3 bis 4 mm Knochenbreite eingesetzt wurde, sowie zwei weitere Fälle zu Illustrationszwecken. Zudem wird die Präparation des rechteckigen Implantatlagers mit der Perforations- und der Expansionstechnik dargestellt. Die klinischen Ergebnisse zeigen (1) eine gute Implantatstabilität mit Stabilisierung tief im Kammknochen, (2) eine periimplantäre Knochendicke von mehr als 1 mm auf der vestibulären und oralen Seite und (3) eine deutlich reduzierte Morbidität, da das neue Implantat die Versorgung schmaler Kämme ermöglicht und damit die Notwendigkeit von Knochenregenerationsmaßnahmen sowie die mit ihnen verbundene Morbidität reduziert.
Manuskripteingang: 19.03.2021, Annahme: 11.05.2021
Schlagwörter: keilförmiges Implantat, piezoelektrisch, schmaler Knochenkamm, minimalinvasiv, horizontaler Knochendefekt, Bone-Splitting
Quintessence International, 5/2020
DOI: 10.3290/j.qi.a44370, PubMed-ID: 32253392Seiten: 406-414, Sprache: EnglischFabrizio, Fontanella / Grusovin, Maria Gabriella / Gavatta, Monica / Vercellotti, Tomaso
Objective: The aim of this randomized controlled clinical study was to evaluate the efficacy of a new technique fully based on the use of a piezoelectric device for third molar root extraction versus the conventional technique based on the use of manual and rotary instruments.
Method and materials: Patients referred to the hospital of Bolzano for third molar extraction were randomly divided into two groups and treated by two experienced oral surgeons. In the test group all the procedures were performed using piezoelectric instruments and a specially designed piezoelectric lever, whereas in the control group conventional manual and rotary instruments were used. The main outcome measure was patient's pain perception, and the secondary outcome measures were complications, duration of the surgical treatment, and soft tissue healing. The study had a 1-week follow-up.
Results: Fifty patients (23 females and 27 males) out of 90 were included in the study, and 100 third molars (50 maxillary and 50 mandibular) were extracted. All patients completed the expected follow-up. No differences were found between the two groups regarding patient's pain perception, complications, and soft tissue healing. However, the new piezoelectric extraction technique took less than half the time when compared to the conventional technique (4.6 ± 4.5 minutes versus 10.2 ± 13.1 minutes; P = .049).
Conclusions: The new piezoelectric third molar root extraction technique allowed third molar extraction in less than one half the surgical time required by the traditional technique. The advantages seem to be more pronounced in difficult cases. However, both surgeons who performed the procedures were very experienced and all the patients were young. Therefore, caution should be given to the generalization of the results. Multicenter studies with a larger variety of patients are needed to confirm the promising results of this study.
Schlagwörter: extraction, oral surgery, piezoelectric, randomized clinical trial, third molar
International Journal of Oral Implantology, 3/2020
PubMed-ID: 32879928Seiten: 235-239, Sprache: EnglischBassi, Francesco / Cicciù, Marco / Di Lenarda, Roberto / Galindo Moreno, Pablo / Galli, Fabio / Herford, Alan Scott / Jokstad, Asbjørn / Lombardi, Teresa / Nevins, Myron / Sennerby, Lars / Schierano, Gianmario / Testori, Tiziano / Troiano, Giuseppe / Vercellotti, Tomaso / Stacchi, Claudio
Purpose: Piezoelectric bone surgery was introduced into clinical practice almost 20 years ago as an alternative method for cutting bone in dental surgical procedures, in an attempt to reduce the disadvantages of using conventional rotary instruments. The aim of this Consensus Conference was to evaluate the current evidence concerning the use of piezoelectric surgery in oral surgery and implantology.
Materials and methods: Three working groups conducted three meta-analyses with trial sequential analysis, focusing on the use of piezoelectric surgery in impacted mandibular third molar extraction, lateral sinus floor elevation and implant site preparation. The method of preparation of the systematic reviews, based on comprehensive search strategies and following preferred reporting items for systematic reviews and meta-analyses (PRISMA) guidelines, was discussed and standardised.
Results: Moderate/low evidence suggests that piezoelectric surgery is significantly associated with a more favourable postoperative course (less pain, less trismus) after impacted mandibular third molar extraction than conventional rotary instruments. Moderate evidence suggests that implants inserted with piezoelectric surgery showed improved secondary stability during the early phases of healing compared with those inserted using a drilling technique. Strong/moderate evidence suggests that piezoelectric surgery prolongs the duration of surgery in impacted mandibular third molar extraction, sinus floor elevation and implant site preparation, but it is unclear whether the slight differences in duration of surgery, even if statistically significant, represent a real clinical advantage for either operator or patient. Weak evidence or insufficient data are present to draw definitive conclusions on the other investigated outcomes.
Conclusions: Further well-designed trials are needed to fully evaluate the effects of piezoelectric surgery, especially in implant site preparation and sinus floor elevation.
Schlagwörter: impacted mandibular third molar extraction, implant site preparation, piezoelectric surgery, sinus augmentation, systematic review
International Journal of Periodontics & Restorative Dentistry, 1/2019
DOI: 10.11607/prd.3219, PubMed-ID: 29677223Seiten: 115-121, Sprache: EnglischSchierano, Gianmario / Vercellotti, Tomaso / Modica, Fabio / Corrias, Giorgia / Russo, Crescenzo / Cavagnetto, Davide / Baldi, Domenico / Romano, Federica / Carossa, Stefano
This retrospective study evaluated implant survival rate (SR) and marginal bone loss around dental implants placed with ultrasonic implant site preparation. A total of 156 implants were placed in 28 totally and partially edentulous patients. Bone loss was measured on intraoral paralleling digital radiographs taken at the impression phase and after 4 years of loading. As 3 implants (1.92%) failed at the second surgery stage, the SR was 98.08% after 4 years. The mean marginal bone loss was 0.52 ± 0.33 mm (0.51 ± 0.35 mm mesially and 0.53 ± 0.35 mm distally), with comparable values for implants inserted into the maxilla (0.52 ± 0.32 mm) and the mandible (0.52 ± 0.35 mm).
The International Journal of Oral & Maxillofacial Implants, 3/2018
Online OnlyDOI: 10.11607/jomi.6270, PubMed-ID: 29763506Seiten: e67-e71, Sprache: EnglischPellegrino, Gerardo / Tarsitano, Achille / Taraschi, Valerio / Vercellotti, Tomaso / Marchetti, Claudio
Zygomatic implant site preparation could be considered a challenging procedure because of the use of a very long twist drill that could sometimes be difficult to control due to the need for drilling the malar bone on an oblique surface. Ultrasound was recently suggested to achieve better control, but the specific long tips required are not readily available, and the elongated tip also tends to reduce the efficacy. This technical note describes a proposal of a novel computer-aided technique to simplify the procedure of zygomatic implant site preparation. This method uses a standard-length ultrasonic tip to prepare the crestal bone and the zygomatic bone in two individual steps. The desired implant trajectory can be achieved during preparation using a real-time tracking navigation system. The combined use of the navigation system and the ultrasonic tips could aid the surgeon, during the first steps, in achieving optimal control of the instruments employed for the implant site preparation and keeping the planned zygomatic implant position. If the efficacy of the procedure is confirmed through clinical trials, this technique could also contribute to reducing the invasiveness of the procedure, promoting a smaller flap, and reducing the soft tissue damage.
Schlagwörter: 3D implant positioning, dynamic navigation, image-guided surgery, navigation system, piezoelectric surgery, zygomatic implant
The International Journal of Oral & Maxillofacial Implants, 3/2017
Online OnlyDOI: 10.11607/jomi.5800, PubMed-ID: 28494042Seiten: e161-e165, Sprache: EnglischPellegrino, Gerardo / Taraschi, Valerio / Vercellotti, Tomaso / Ben-Nissan, Besim / Marchetti, Claudio
This case report describes new implant site preparation techniques joining the benefits of using an intraoral navigation system to optimize three-dimensional implant site positioning in combination with an ultrasonic osteotomy. A report of five patients is presented, and the implant positions as planned in the navigation software with the postoperative scan image were compared. The preliminary results are useful, although further clinical studies with larger populations are needed to confirm these findings.
Schlagwörter: anatomical preservation, image-guided surgery, oral implantology, osseointegration, piezoelectric surgery, 3D implant positioning
International Journal of Periodontics & Restorative Dentistry, 1/2014
DOI: 10.11607/prd.1860, PubMed-ID: 24396835Seiten: 10-18, Sprache: EnglischVercellotti, Tomaso / Stacchi, Claudio / Russo, Crescenzo / Rebaudi, Alberto / Vincenzi, Giampaolo / Pratella, Umberto / Baldi, Domenico / Mozzati, Marco / Monagheddu, Chiara / Sentineri, Rosario / Cuneo, Tommaso / Di Alberti, Luca / Carossa, Stefano / Schierano, Gianmario
This multicenter case series introduces an innovative ultrasonic implant site preparation (UISP) technique as an alternative to the use of traditional rotary instruments. A total of 3,579 implants were inserted in 1,885 subjects, and the sites were prepared using a specific ultrasonic device with a 1- to 3-year follow-up. No surgical complications related to the UISP protocol were reported for any of the implant sites. Seventy-eight implants (59 maxillary, 19 mandibular) failed within 5 months of insertion, for an overall osseointegration percentage of 97.82% (97.14% maxilla, 98.75% mandible). Three maxillary implants failed after 3 years of loading, with an overall implant survival rate of 97.74% (96.99% maxilla, 98.75% mandible). (Int J Periodontics Restorative Dent 2014;34:11-18. doi: 10.11607/prd.1860)
International Journal of Periodontics & Restorative Dentistry, 4/2007
PubMed-ID: 17726988Seiten: 324-331, Sprache: EnglischVercellotti, Tomaso/Podesta, Andrea
Eight patients with malocclusions were treated with a new orthodontic-surgical technique that reduces the duration of treatment compared to conventional techniques. The monocortical tooth dislocation and ligament distraction (MTDLD) technique combines two different dental movements that work separately but simultaneously on opposite root surfaces. On the root surface corresponding to the direction of movement, vertical and horizontal microsurgical corticotomies are performed around each tooth root with a piezosurgical microsaw to eliminate cortical bone resistance. The immediate application of strong biomechanical forces produces rapid dislocation of the root and the cortical bone together. On the root surface opposite the direction of movement, the force of dislocation produces rapid distraction of ligament fibers. During the osteogenic process that follows, application of normal orthodontic biomechanics achieves the final tooth movement. All eight patients underwent periodontal and radiologic examinations for more than 1 year after treatment. No periodontal defects were observed in any of the patients, including one with a severe malocclusion and a thin periodontal tissue biotype. Compared to traditional orthodontic therapy, the average treatment time with the MTDLD technique in the mandible and maxilla was reduced by 60% and 70%, respectively.
International Journal of Periodontics & Restorative Dentistry, 6/2005
Seiten: 543-549, Sprache: EnglischVercellotti, Tomaso/Nevins, Marc L./Kim, David M./Nevins, Myron/Wada, Keisuke / Schenk, Robert K./Fiorellini, Joseph P.
A piezoelectric instrument vibrating in the ultrasonic frequency range was investigated for its potential use in periodontal resective therapy. The rate of postoperative wound healing (baseline and 14, 28, and 56 days after surgery) in a dog model following surgical ostectomy and osteoplasty was the marker used to compare the efficacy of this instrument (PS) with a commonly used carbide bur (CB) or a diamond bur (DB). The surgical sites treated by CB or DB lost bone, in comparison to baseline measurements, by the 14th day, while the surgical sites treated by PS revealed a gain in the bone level. By day 28, the surgical sites treated by all three instruments demonstrated an increased bone level and regeneration of cementum and periodontal ligament. However, by day 56, the surgical sites treated by CB or DB evidenced a loss of bone, versus a bone gain in the PS-treated sites. Thus, it appears that PS provided more favorable osseous repair and remodeling than CB or DB when surgical ostectomy and osteoplasty procedures were performed. Therefore, PS could be regarded as being efficacious for use in osseous surgery.